This blog is to help the medical community understand the Alexander Technique.
I do not think it is the responsibility of the AT community to help raise the awareness of the AT in the medical community. It is the the responsibility of the medical community to practice evidence based medicine and to choose interventions which are effective and safe. That they have ignored the AT since the BMJ study is one of the greatest medical errors of modern time.
That being said, as an emerging Alexander Technique professional I want to help the AT community to relate more effectively with the medical community. I've written them this entry:
In my nearly three years of training to become a teacher I have been very impressed with the wide ranging benefits that students in the AT can expect. One of the most perplexing questions surrounding the Alexander Technique is “Why is it not more popular?”
All AT professionals come to the AT from particular groups and backgrounds. We naturally see the benefits and potentials of the AT in terms of our history. Having spent the past 15 years in the medical field, I tend to focus of the benefits that the AT could provide for the patients. If the medical profession recommended the AT, their patients would benefit, but it is also important to note that medicine is influential in the broader culture as well. So why doesn’t the medical profession recommend the AT?
I think much of the blame can be placed at the feet of the medical care establishment. It is their job to diagnose a condition and then recommend interventions that are safe, effective and within the patients means. That they have not been recommending the AT is rather damning.
But is the entire blame to be placed on the medical community for their lack of appreciation of the benefits of the AT? Could the AT community be approaching the medical community in a more effective manner?
At the last ACGM, I was bemoaning to one my betters the fact that so few medical professionals recommended the AT. He replied that if we could only get our hands on more doctors they would be very happy to support us. Indeed, this was the practice of Alexander himself and he was very effective. But this approach no longer seems to work. The AT is stuck in an obscure corner of “alternative therapies” with few sign of expanding to it’s potential. Are we just not trying hard enough? After 100 years is it time to try something different?
This article discusses some possible reasons why we have been ineffective, and suggests a change in course.
To be honest, I’m being unfair. Just the continued existence of the technique says quite a bit about it’s efficacy. Scores of Great Ideas have caught the publics attention over the past 100 years. Sooner or later they’ve all faded into the background. But the AT has persisted. This says quite a bit about it’s benefits and about the quality of it’s teacher training programs.
That the AT continues to exist does not dilute my central thesis: the AT has not grown to it’s potential in the healthcare setting. Pain is the most common complaint in the medical setting and chronic back pain is the most common type of chronic pain. Yet the medical community has little that is safe and effective for chronic back pain. For this reason, there is an acupuncturist, a chiropractor and a massage therapist are on every corner. Why is the AT nearly invisible?
CAN WE TALK TO DOCTORS?
My bosses boss was the first doctor I spoke with about training to be an AT teacher. I opened my pitch saying that I wanted our organization to help pay for my AT teaching program. I had not gotten past this first sentence when he stopped me and spoke for about 2 minutes without stopping. Of course, he had never heard of the AT. But in those two minutes he told me three times that he was ”openminded”. I knew I had my work cut out for me!
Physicians have several barrier to understanding the AT. They have a very strong tendency to try to fit anything new into their existing paradigm. The medical view is quite different from the AT world view. For example, they help others by recommend therapies and prescribe treatments. That the AT is an educational technique is confusing to them. Next, the therapies prescribed by physicians have very narrow indications. They will assume any intervention will only help a narrow population with a very specific illness. Finally, the notion that it is always useful to fragmented the self into not only the body and mind but into specific organ systems is utterly unchallenged.
In addition to the fundamental differences we have with the medical profession, we can expect that the medical professional will immediately lump the AT in with all the other new age, alternative, Next Big Things which are constantly being thrown at the physicians. Physicians grow fatigued responding to these “Great Ideas” which generally have unproven benefits and are both expensive and dangerous. Further, they are promoted without reference to the life sciences or the scientific method which form the bedrock of medicine. It is not surprising that medical professionals are impatient and reflexively sceptical of anything new.
WHAT IS THE ALEXANDER TECHNIQUE?
It’s a sure bet it will be among the first questions the physician might ask. Like any other encounter, the first moves are crucial. Very soon the conversation will turn to the specifics and studies. I take the opportunity to start dissolving the assumptions physicians are sure to have.
Well, I think it’s very important to understand the the Alexander Technique is an educational technique, not a therapy.
As an educational technique, a variety of benefits can be expected. Also, I’m not claiming cures and miracles. If a medical provider can not imagine anything other than a therapy might possibly be helpful, I might make the analogy to nutrition.
The Alexander Technique helps students make changes at a pretty fundamental level. Some people use the analogy of nutrition. If you send an patient who eats fast food and has high cholesterol to a nutritionist, and they make the changes that the nutritionist suggest, then you can expect fundamental changes to a lot of ailments. But nutrition is not a specific therapy for high cholesterol. Good nutrition is fundamental to living well. Of course, the AT has nothing whatever to do with eating, but both are educational interventions.
“OK, the Alexander Technique is some kind of educational technique, but what is it exactly?”
“Oh, I can tell you. But is that what you really want to know?”
WHAT DOES A MEDICAL CARE PROVIDER REALLY WANT TO KNOW?
Physicians want to provide the best possible care. How do they decide what to recommend? In ancient times doctors relied on tradition or religious beliefs.
In FM Alexander's time medical professionals placed emphasis on expert opinion and the consensus among elders. Alexander realized this and was very successful by seeking out the most influential medical professionals of his time.
But in modern times we have moved well beyond relying on ‘tradition’ or the ‘consensus of experts’. Currently, physicians are taught to be suspicious of tradition, expert opinion and community standards. Moreover, physicians are taught to discount their own experiences and those of their colleagues.
So how does the contemporary medical community decide what care is best? How do they decide what to recommend?
“Oh, I can tell you what the Alexander Technique is, but is that what you really want to know? Do you know the story of penicillin? Prior to the discovery of penicillin blood poisoning (sepsis) was nearly always fatal. But then it was found that the mold from bread, when refined, was safe and effective in curing sepsis! But for 40 years no one knew exactly why this was so. No one knew the mechanism by which it worked. Those physicians who started to use penicillin when it was found to be safe and effective saved their patients. Those physicians who waited till they figured out how penicillin worked lost many patients during those years.
Sure, I can explain how the AT works, but is that what you really want to know? Don’t you want to know what evidence is there to suggest that the AT is safe and effective?”
BUT SAFE AND EFFECTIVE FOR WHAT?
The fact is, of course, we have no idea what the boundaries of the benefits are with the AT. All the studies are encouraging but there are whole fields of human endeavor where the AT has not been studies. The best study to date has to do with chronic back pain.
The primary care physician will be very interested in this. Back pain is among the most difficult problems physician face. Although back pain is a leading cause of chronic pain, disability, and medical visits, physicians have not identified any cause. Only fifteen percent of back pain has an identified cause. Because physicians have not found a specific cause to the remaining 85% they call it “non specific”.
Until recently modern day physicians were taught to aggressively treat pain. Since narcotic were shown to be helpful in the short term, they became very popular as a treatment for long term “nonspecific” back pain. Recently they have been found to be neither safe nor effective for chronic pain. So physicians are desperate for anything that is safe and effective for back pain.
HOW DO MEDICAL CARE PROVIDERS DECIDE WHAT RECOMMENDATIONS TO MAKE?
This is a highly controversial topic and there is heated debate with medical, legal, ethical and economic considerations. But there is evolving consensus within the medical community to rely on population based evidence when caring for the individual. This means that the medical provider is encouraged to look to scientific studies of large numbers of people who are similar to their patient for guidance when prescribing care.
The stratification of the quality of evidence that a treatment is effective is important. There are two bodies have have been created to give grades to the quality of evidence - or level of certainty - that an intervention is effective. These two bodies are the US Preventative Service Task Force, and the UK National Health Service. The US Preventative Task Force defines the lowest level (Level III) of evidence to the opinions of respected authorities. So much has changed since FM’s days when this was the best available evidence! The highest level (Level I) is given to “Evidence obtained from at least one properly designed randomized controlled trial.”
Again, more than any other criteria, physicians want to know that an intervention is safe and effective. We now have a definition about what is thought to be effective, but how does safety come into equation? Again, the US Preventative Task Force has tried to lend guidance. They have summarized both the quality of the evidence - and dangers - of an intervention in their “Categories of Recommendation”. The top level is Level A: “Good scientific evidence suggests that the benefits of the clinical service substantially outweigh the potential risks. Clinicians should discuss the service with eligible patients.”
“After lessons in the Alexander Technique one can expect a variety of benefits. The BMJ study suggests that it is highly effective in the long term relief from back pain. In fact, it is the highest quality evidence: Level I. And because there was no unwanted effect from the Alexander Technique it should have your top recommendation. Right?”
There only remains one problem, and that is that we only have this one top quality study. Physicians feel much more confident when they have several top quality studies with similar conclusions. After admitting this, one can feel free to add:
“- The number of participants in the BMJ study were huge - bigger than some meta studies of other interventions.
- It was sponsored by the British NHS who had a genuine interest in an unbiased outcome.
- It was consistent with other AT studies that show the AT is very effective.
- The benefits did not wear off as time went on like everything else that has been studied. In fact, the benefit from the AT was actually better at 12 month follow up than it was 6 months.
- The reduction in days in pain, one of the two primary outcomes, was huge: an 86% reduction compared to the control group. The other primary outcome, disability, showed a 42% reduction. The secondary outcomes also showed very impressive benefits.
-Sure, subsequent studies may show less benefit, but what is the chance, given the size, quality, and magnitude of benifit that subsequent studies with prove that there is no benefit?
- Oh, and did I mention that this is 100% safe?
HOW DOES THE ALEXANDER TECHNIQUE HELP WITH BACK PAIN?
Ultimately, medical providers are human and curious, and want to understand the underlying mechanisms. Although I’ve argued that physicians should not predicate their recommendation based on an understanding of how the technique works, it’s not unreasonable for them to ask how it works. An easy response would be to simply quote the BMJ study it self:
“Lessons in the Alexander technique offer an individualised approach designed to develop lifelong skills for self care that help people recognise, understand, and avoid poor habits affecting postural tone and neuromuscular coordination. Lessons involve continuous personalised assessment of the individual patterns of habitual musculoskeletal use when stationary and in movement; paying particular attention to release of unwanted head, neck, and spinal muscle tension, guided by verbal instruction and hand contact, allowing decompression of the spine; help and feedback from hand contact and verbal instruction to improve musculoskeletal use when stationary and in movement; and spending time between lessons practising and applying the technique (also see appendix on bmj.com).”
This is a convenient and easy-to-understand definition. And the claim that the AT improves postural tone and neuromuscular coordination is supported by other studies. But as a definition of the AT I do not think it is very complete.
One of the overarching themes in FM writing is that that is not useful to divide the mind and the body. This is not some abstract theory. It is the reason some teachers, like Becca Furguson, have been using the AT to help students with anxiety, trauma and PTSD. Lessons in the AT lead to more than just changes in muscular tone. But how do we explain all this to medical care provider whose paradigm is so different than our own?
WHAT IS PAIN?
When physicians gather to talk about medical problems, they first define the problem. The definition of pain, and the theory about how it is created, has changed quite a bit over the years. In ancient time, pain was thought to be evil spirits entering the victim. With the advent of religion, pain was thought to be a test of ones faith, and treatment involved prayer and devotion. Our culture is heavily influenced by Descartes who gave us a mechanistic, dualistic perspective. Descartes suggested that pain was trauma or inflammation in the periphery, triggering pain receptors, traveling through pain pathways to a pain center in the brain. But we now know there is no pain center in the brain: pain is a widespread phenomenon. Also, years of cutting nerves thought to carry of pain rarely result in long term pain control.
Ronald Melzac, a Canadian researcher, developed the “gate control” theory of pain. He hypothesized that a ‘gate’ in the spinal cord inhibits, allows or amplifies the transmission of pain from the periphery. In the model, inputs to the gate from the brain can descend the spinal cord and effect this spinal gating mechanism. This model is now generally accepted.
The progression in pain theory from early times to modern time is marked by increasing participation of the sufferer: from victim to active participant. And the cause of pain has moved from outside the body, to the periphery and now more centrally.
However, the gate control theory does not account for a common finding called phantom limb pain. This is when people feel pain in a non-existent limb: It is common for people to feel pain in a limb that was amputated. Even more puzzling is the perception of pain in a limb in a person that was not born with the limb.
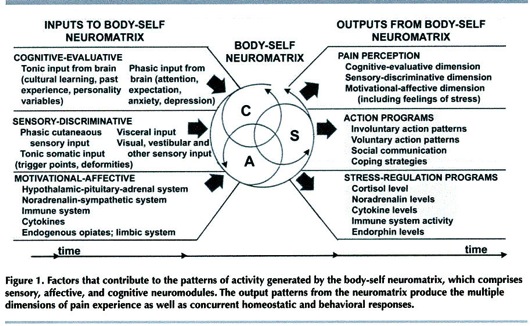
To explain this, Ronald Melzac has proposed another revision to pain theory. This one is called the “body-self neuromatrix” (BSN). This theory is bit complicated but well worth the effort to study it. The BSN theory states that there is a widespread scaffolding or lattice of neurons that extend throughout the brain. One is born with this matrix, but it can be modified during one's life. This matrix has a variety of inputs and outputs and the specifics of it’s workings are very complicated. However, it has two functions. First, it decides if the ‘self’ is OK or Not OK - it decides if equilibrium, or homeostasis, is preserved or lost. The second function is that the BSN generates a constant neural stream that goes to the “sentient neural hub” where it is converted to a continually changing stream of awareness.
Melzac, a psychiatrist by training, divides the inputs to the BSN into three categories: the mind (thoughts, beliefs, history, culture, anxiety, etc), body (somatic sensation such as trauma, trigger points, tonic state, sight, sounds, etc) and from the endocrine system (stress hormones, immune system, etc). All these inputs can contribute to the loss of homeostasis, and can destabilize the body-self neuromatrix.
Melzac groups the outputs from the body-self neuromatrix into three categories. These three outputs include the creation of the perception of pain and stress, changes to one’s actions (coping activities such as voluntary and involuntary actions, social interactions, etc) and body (stress hormones, changes to the immune system, etc).
Again, I believe this theory can be very helpful to anyone cares for those with chronic pain, or anyone at risk of having pain. Here are some points I’d like to emphasize:
-Pain is created in the mind. Pain is a psychological phenomena. Somatic stimuli can contribute to the perception of pain, but these stimuli are not the pain, and are not necessary for the creation of pain. So, one’s chronic back pain may, or may not, have anything to do with one’s back.
-Pain is not an isolated phenomena. It is only one of the outputs from the BSN that affects the entire self. The other outputs are very important and can lead to a wide array of serious psychological and interpersonal problems, as well as endocrine, inflammatory and immunologic diseases.
-This theory appears to be a fragmentation of the self, something we view as not very helpful. But the medical professional that adopts this model will be forced to recognize the contribution of the entire self in the creation of pain. Also, the medical professional will be forced to acknowledge that loss of homeostasis results in widespread harm to the entire self and not simply the creation of pain. In fact, some believe that the notion of “pain” unduly narrows the attention of both patient and medical provider, and diverts attention away from other very serious disruptions. Some believe the the notion of pain is obsolete and should be replaced with a more inclusive term.
-Melzac proposes this is a linear process: input, processing in the BSN, and then output. But clearly, it is not this simple. The outputs from the BSN will effect the next cycle. For example, the startle reflex (like other reflexes) is a brainstem reflectory process and does not have cortical (thought, memory, beliefs, etc) participation - this is what Magnus found. But within a few milliseconds the repercussions of the startle reflex itself will influence the BSN. What we observes, then, in the startle response is the sum of the startle reflex plus the stability, or lack of stability, of the BSN.
-This theory does more than explain how pain is created. It also explains how PTSD and anxiety are created. Researchers have long noted the connection between post-traumatic stress disorder and chronic pain. With this theory, we no longer have to wonder about the relationship of pain and PTSD: PTSD/anxiety are created by the BSN along with pain.
-Finally, this theory extends the progression of pain theory. Originally pain was thought to be external and victimizing the sufferer. This theory places the creation of pain, not outside or inside the body but in the mind. Hence, the sufferer is not a helpless victim but actually an active participant in the creation of their suffering.
HOW DOES THE AT HELP WITH PAIN?
Now we have a usable theory of what pain is, how it is created and what contributes to pain. This theory can used to discuss the AT and some of it’s mechanisms with the medical community.
In terms of the body self neuromatrix, I suggest that the AT works in the following ways:
1. The AT affects the phasic (ie., rapid, transient) state of the mind. The tool of inhibition can be used to stop the perseveration and catastrophizing that are common responses to somatic sensations. This is not distraction. This is consciously attending to the wide variety of inputs - our entire sensory environment - rather than attending solely to the habits of mind.
2. The AT affects the phasic somatic inputs. Acute injury and emotional trauma are strong stimuli to the BSN and strong stimuli to pull down and shorten in the characteristic pattern seen in the startle response. The tools of the AT have the potential to prevent this response. If we can prevent this characteristic response, then the BSN will be confronted with a discordance: in the moments following significant trauma, there will not be the characteristic phasic somatic input (ie. no shortening and contracture) input to the BSN. It does not change the trauma, but it does change our response to it. The quality of the experience will be different and less likely to cause suffering.
One curious finding in the BMJ study is difference in the magnitude of the effect in the two primary outcomes: days in pain and disability. The percent reduction in days in pain (86%) was over twice the reduction in disability (42%). There may be any number of reasons for this disparity. One reason might be that many participants may well have continued to have problems with their back a year after the intervention. The somatic sensations that accompany such activities as chores around the house, may prevent them from doing the chores. This would lead to less reduction in the disability score. But if these same somatic sensations were not accompanied by the characteristic changes that always accompany pain (shortening and narrowing), the BSN will be stabilized and not prompted to create the sensation of pain. This would lead to a greater reduction in days with pain.
3. The AT affects the tonic state of the mind. Some have noted the similarities between the AT and mindfulness meditation. Becca Furguson goes so far as to refer to the AT as “movement based mindfulness”. This is important because meditation is known to make the mind less reactive. As such, meditation holds great promise in helping those with PTSD and pain, and “mindfulness based therapies” are very popular.
Meditation is gathering the mind. But if we look closer it’s really a two step process. The first is to recognize and stop the distracted mind. This then allows the meditator to come back into the present. The second step to focus on the object of meditation. This second step, “focusing”, is optional but generally recommended.
FM used only slightly different language. His “inhibition of end gaining” is to continually say no to caring more about getting to an end than about how one gets there. This ‘end gaining’ seems the same as getting ahead of oneself and is similar to ‘not being present’. This ‘inhibition of end gaining’ is the same activity as the meditators first step: coming back to the present. The main difference is not the activity, but the context: the meditator aims to ‘be present’ on the meditation cushion while the AT student intends to ‘inhibit end gaining’ in all activity.
Mediation is known to help those suffering from pain, anxiety and PTSD. The BSN theory predicts that it should be helpful. We can argue that the AT will have even more benefit than meditation: inhibition is taught as the response to all stimuli to act throughout the day, and not practiced only once or twice a day.
4. The AT affects the tonic somatic inputs. The AT improves postural tone and spinal coordination. This was used as a definition of the AT in the back pain study cited above, with evidence provided by Dr. Tim Caccitore. This improved tone is relayed to the BSN and will decrease tonic inputs. This improved tone is not consistent with loss of homeostatis - it is consistent with stability.
In addition, it’s reasonable to assume the improved tone and spinal coordination - a “healthy back” - should help prevent future injuries.
CONCLUSION
For the past 100 years, little progress in communication has occurred between the AT community and medicine. Meanwhile back pain sufferers have little hope and the AT remains in the shadows. Waiting for the medical community to come to us is obviously not working. It is time to try something else.
There are risks in engaging the medical community, as FM clearly perceived. The medical establishment can be expected to relate to the AT in procrustean terms, ignoring or trivializing central points that do not fit the medical paradigm. Any equivocation or simplification on the part of the AT community will result in the AT being defined as a therapy with narrow indications. I believe it is important to have a robust platform from which to discuss the AT in be broadest possible terms.
Although there is a great divide between the medical care paradigm and the AT community, it does not mean that we can not find common ground. We both have inter-relating unmet needs and solutions. For example, medical care providers are desperate to find anything that will help with chronic back pain but they require scientific proof of safety and efficacy. The AT community has excellent, but not complete, science to support it, and a stellar safety record. We all can also discuss how the AT works using modern pain theory.
We must understand the medical mind and appeal to it in it’s terms. This means understanding and speaking clearly about science and logic. This is not a small task for the AT community whose roots tend to be in the performing arts - a group not known for it’s firm grasp on logic, biological science and statistics. But if we understand how medical decisions should be made, our task is much easier. We do not have to explain how, exactly, the AT works. “How” is not a logical consideration when recommending the AT.
The AT community needs be clear only on two points. First, nothing other than the AT has been shown to be significantly effective in non-specific back pain in the long term. Of course, the studies on the AT are not conclusive. But there is almost no medical problem where the evidence to recommend an intervention is unequivocal. Almost nothing in medicine is black and white. In this grey zone, medical recommendations should be heavily influenced by safety: first, do no harm. This is the second of the two points at which the AT community must be clear when talking with the medical community: There has never been an unwanted outcome - there has never been any harm - in any study involving the AT.
And yet, the medical community is curious and will want to know how the AT works. By what mechanism does the AT help with pain? We can not use old theories of pain. Most medical care providers have simplistic, unexamined assumptions about the nature of pain based on ancient, incorrect assumptions regarding the nature of the Self. It is not surprising then that their efforts, based on these false assumptions, have not yield an effective therapy for chronic back pain. Also, these older theories do not give us the possibility to have a full discussion regarding the mechanisms by which the AT works.
The good news is that advances in pain theory are starting to re-integrate the fractured self. Modern pain theory provides the opportunities to discuss not only the effects of improved postural tone and spinal coordination, but improved phasic response to otherwise disruptive somatic stimuli, interrupting the undue fear response, the psychic perseveration and the catastrophization. And in the same discussion about the mechanism by which the AT helps with pain, we can discussed how the AT will help with other problems, such as PTSD and anxiety.